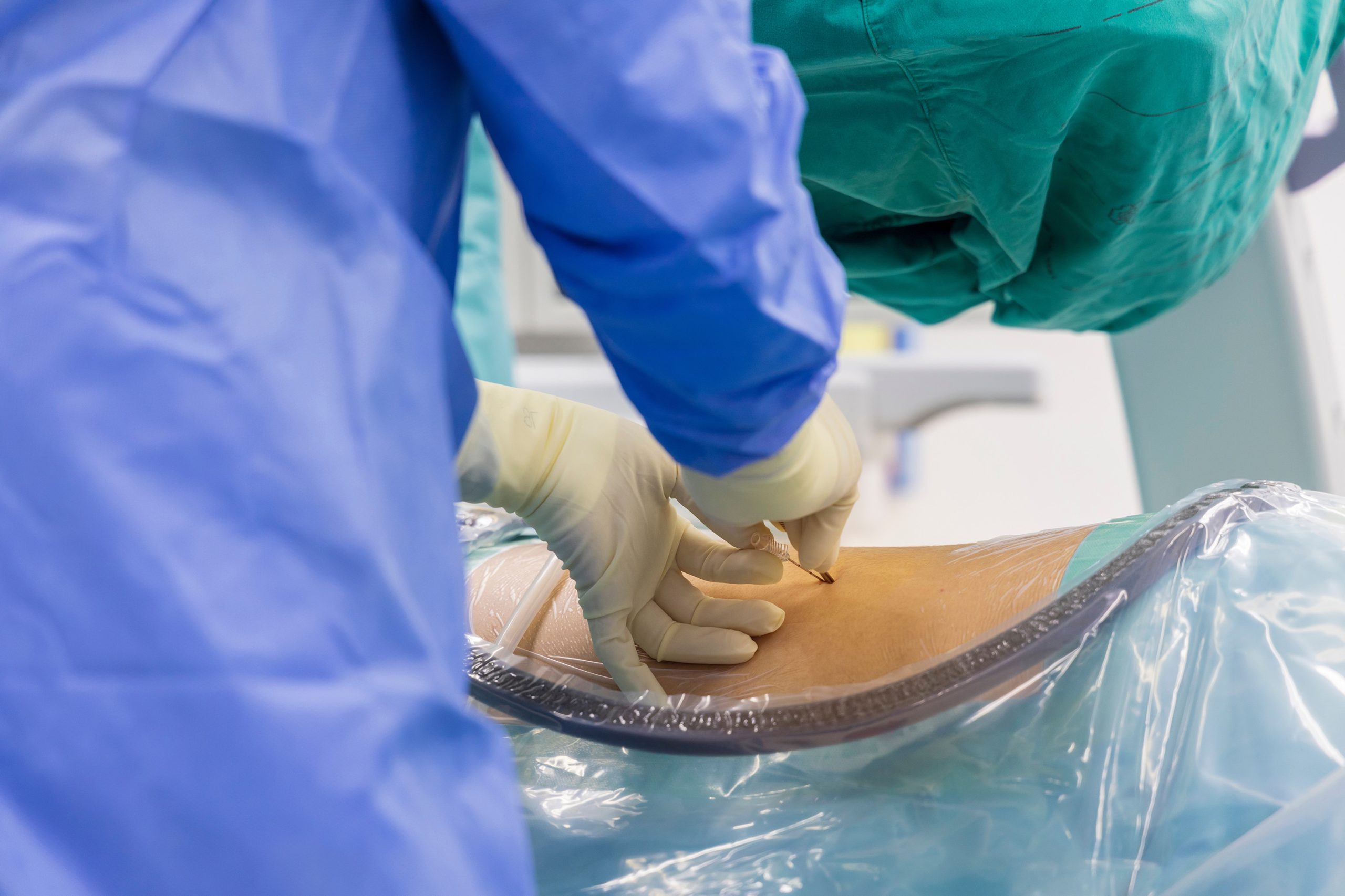
Epidural Steroid Injections
Epidural Steroid Injections (ESI) can help alleviate the pain you experience in your lower back/legs, mid-back and neck/arms. These injections tend to be very helpful with what is known as radicular (pain in the arms or legs) symptoms or “nerve pinching.” These can be done in different areas of your spine:
- Lumbar epidural steroid injection. This is used for the treatment of low back pain, such as spinal stenosis, sciatica, radiculopathy, herniated discs, degenerative disk disease etc.
- Thoracic epidural steroid injection. This is used to treat the same problems mentioned above, but in the mid-back area.
- Cervical epidural steroid injection. This is the same procedure mentioned above but done in the neck.
There are two different types of Epidural Steroid Injections, one is called interlaminar (or translaminar), and the other one is the transforaminal. Both are very successful in the treatment of the above-mentioned problems.
Candidates for Epidural Steroid Injections
Candidates for epidural steroid injections have back pain, and/or pain radiating down the arms and legs. Pain relieved by ESIs can be the result of many conditions, including the following:
- Lumbar-disc herniation
- Degenerative disc disease
- Lumbar spinal stenosis
- Vertebral compression fractures
- Cysts in a facet joint or nerve root
- Annular tears
Epidural steroid injections can be used alone to provide pain relief, or given as part of a rehabilitation program to help a patient perform physical therapy exercises with less discomfort. Relief from a single injection can last from 1 week up to 1 year; a typical positive response lasts for 1 month. If helpful, injections can be repeated at 2-week intervals, but usually no more than 3 or 4 times per year. ESIs can also be of diagnostic value in pinpointing the source of the pain and determining its severity, which can assist a physician in developing an appropriate treatment plan.
The Epidural-Steroid-Injection Procedure
Epidural steroid injections are administered by many types of physicians, including anesthesiologists, orthopedists, physiatrists, pain-management specialists and neurologists. Typically, they are administered in an outpatient facility, under the guidance of fluoroscopy, to verify that the medication is reaching the inflamed nerve root. Because the injection contains a local anesthetic as well as a corticosteroid, the injection is not usually painful, although a patient may feel pressure at the injection site. The injection procedure takes only a few minutes.
In most cases, the patient experiences immediate pain relief due to the anesthetic, but the relief is temporary and wears off in a few hours. During the next day or two, however, as the corticosteroid works to reduce inflammation, the patient should feel a significant, if not total, alleviation of pain. The patient can usually resume normal activities the day after the procedure.
Additional Resources
No. The procedure may lessen your pain, facilitating participation in physical therapy. The amount of relief and duration of relief is patient dependent.
Yes, ESI is very safe, but as with any other medical procedure, it has risks. The most common complication is a headache. Other more serious complications, such as infection, allergic reaction, nerve damage, bleeding and paralysis can occur, but are extremely rare. The steroid can cause some fluid retention, facial flushing, and can raise blood pressure and blood sugar levels. Talk to your physician about how to manage these side effects.
First the skin will be cleaned with a special solution. This will feel cold. Then your skin will be numbed with a local anesthetic. This will induce a stinging and burning sensation for a few seconds. During the Epidural Steroid Injection, a small needle is placed and advanced into the epidural space under live fluoroscopy. Since the skin is numb from the local anesthesia, you might feel mild discomfort or pressure. The time required to do the procedure varies from patient to patient, but usually takes 10-15 minutes.
As soon as possible. The staff in the clinic will provide you with care instructions after the injection. Please follow them. We recommend that you continue your normal activities as soon as the next day. It is very important to keep your body active.
Yes, but as previously mentioned, complications might occur, as well as side effects from the steroids. The most common complication is a headache is a specific type of headache. It normally improves with time, hydration, and rest. If this happens you should contact our office. Another common complication is infection; we recommend that you shower or bathe the morning of the procedure to minimize risk. Other more serious, but very rare complications can occur, such as nerve damage, meningitis, bleeding or paralysis. Our staff will discuss in detail the risk and benefits before scheduling this injection.
The procedure is intended to decrease your pain. Should you not respond to injections and MRI reveals a surgical pathology, the patient can be referred for a surgical consultation.
If you had no relief from the first injection, you should be evaluated to discuss further interventional therapies. In some cases, a different level, approach, or medication can be used.
There are other therapies that can be used to manage pain. Using different methods to treat your pain is the most successful way to relieve your pain and improve your quality of life. Other strategies to treat your pain include exercise, relaxation, and changing negative behaviors and thought patterns to help you cope with your pain.
• If you are pregnant or breastfeeding.
• If you have a severe allergic reaction to local anesthetics or steroids.
• If you are taking a blood thinner, such as Warfarin (Coumadin), Enoxaparin (Lovenox), Clopidogrel (Plavix), etc; and your medical condition does not allow us to stop it a few days prior to the procedure.
• If you develop a fever or any infection.
• A severe headache
• A fever
• Pain that is more severe than prior to the injection
• Increased back pain or back stiffness
Go to the nearest Emergency Department or call 911 if you develop any new numbness, weakness, and/or paralysis in your arms or legs or lose control of your bladder or bowels.
